Many cases of plantar fasciitis improve with simple home treatments like resting the foot, icing it and using arch supports and over-the-counter pain relievers. If these don’t help, you should see your doctor right away.
Plantar fasciitis treatment Perth can give you corticosteroid injections to ease pain and reduce inflammation. They may also inject platelet-rich plasma (PRP), which contains healing growth factors, into the damaged plantar fascia.

Symptoms
Pain on the bottom of your foot or heel. It usually comes from walking or standing for long periods of time. It may be a dull ache or feel like a sharp stabbing pain. It may be worse in the morning or after long periods of rest. It may also hurt more when climbing stairs or after exercising.
Plantar fasciitis occurs when the plantar fascia (the band of tissue that runs along the bottom of your foot) gets irritated and inflamed. This band of tissue helps to form your arch and connects your heel bone to your toes. It is similar to a rubber band and helps absorb the shock from your feet hitting the ground when you walk or run.
The best treatment for plantar fasciitis is to stop activities that cause pain and to use ice on the affected area several times a day. Medications such as nonsteroidal anti-inflammatory drugs (ibuprofen or naproxen) can help reduce pain and swelling. A physical therapist can teach you exercises to stretch the foot and Achilles tendon. A night splint that holds the foot in a flexed position over the arch during sleep can also help.
If home treatment doesn’t improve your symptoms, you should see a doctor. He or she will ask about your medical history and do a physical exam. The doctor will check for tenderness in the bottom of your foot and look for areas of inflammation. X-rays or ultrasound can show thickening and scarring of the plantar fascia.
Diagnosis
Plantar fasciitis usually results from straining the ligament that stretches from your heel to your toes. One strain probably won’t do much damage, but repeated ones can weaken the ligament and lead to pain. Your Perth podiatrist will diagnose plantar fasciitis by performing a physical exam and checking your symptoms. He or she may also order an X-ray or magnetic resonance imaging (MRI) test to confirm the diagnosis and rule out other conditions, such as a stress fracture or nerve entrapment.
Your doctor may recommend resting your foot by reducing or stopping activities that aggravate the pain. This might include limiting athletic activities that cause your feet to pound on hard surfaces and taking up low-impact exercises such as swimming or cycling. Your doctor may also recommend stretching your foot and calves to help with the pain.
Over-the-counter NSAIDs can help reduce pain and swelling. If NSAIDs don’t help, your doctor might suggest extracorporeal shockwave therapy (ESWT) to stimulate the tissue and encourage healing.
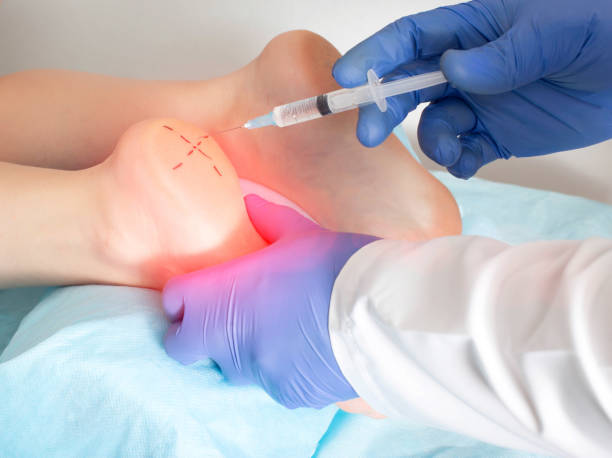
Treatment
The most common symptom of plantar fasciitis is pain that comes on the bottom of your foot, usually in the area of your heel. The pain may be a dull ache or a sharp, stabbing sensation. You may notice that the pain is worse when you first step out of bed in the morning, but it typically lessens or disappears as your feet warm up.
Most people with this condition get better within nine to 12 months after starting simple treatment methods. These include resting the affected foot as much as possible and changing or avoiding activities that cause pain. Using shoe inserts to cushion your feet and reduce stress on your heels is also helpful. Icing the sore spot on your foot several times a day and using nonsteroidal anti-inflammatory drugs (NSAIDs) to decrease pain and inflammation are also recommended.
Your doctor may suggest that you work with a physical therapist on stretching exercises to help stretch your calf muscles and plantar fascia. These exercises should be done several times a day. A physical therapist can also recommend a variety of treatments, including ice treatments and massage therapy, to decrease your pain and inflammation.
If these treatments aren’t effective, your doctor may want to order magnetic resonance imaging (MRI) or ultrasound. These tests aren’t used to diagnose plantar fasciitis but are sometimes ordered if the other treatments don’t help or if your doctor thinks there is another cause of your heel pain.
Prevention
If you’re experiencing pain in your heel or foot that doesn’t get better within a week, talk to your healthcare provider. They can help you find at-home treatments to reduce inflammation and improve your symptoms.
Plantar fasciitis occurs when the dense tissue band that runs along the bottom of your foot irritates or tightens, causing painful heel and arch pain. The pain is usually felt when you stand or walk and can feel like a bruise or an ache. The pain can also be felt when climbing or walking up or down stairs, especially when you’re first getting out of bed or after sitting for a long time.
Prevention options for plantar fasciitis include keeping the calf muscles and Achilles tendon flexible and avoiding overuse of your feet. Adding stretches to your routine can also decrease the likelihood of developing plantar fasciitis, as well as wearing shoes with proper support and making sure your arches aren’t too high.
For those who continue to have heel pain that doesn’t improve with rest and other nonsurgical treatment options, a doctor may recommend a cortisone injection or more intensive therapy. Most people who receive conservative treatments for plantar fasciitis experience improvement within 12 months. For severe cases, surgery may be required.