If you don’t have a website that is modern, attractive and easy to navigate, your clients may find it difficult to connect with your practice. That is why it’s important to understand some basic principles of great web design.
The Hope Therapy Center website shows their patients’ stories to help new visitors build trust. They also offer online appointment scheduling and a lead form for patients to communicate with their office via text message.

Branding
Whether you’re an independent mental health professional or part of a larger healthcare organization, your website plays a critical role in client acquisition. A well-executed healthcare website design showcases your commitment to professionalism, ensuring that prospective clients perceive your brand as trustworthy and reliable, thereby enhancing their confidence in accessing vital information about your practice
When evaluating potential website designers, prioritize those who offer customizable web design elements that align with your specific branding and therapeutic style. A website that reflects the vibe of your practice is more likely to capture a new client’s interest and inspire them to reach out for a consultation.
The layout of your website should also work with the way people read online. Most visitors scan a webpage in an F-based pattern (looking left to right and top to bottom), so it’s important to organize your content in a way that matches their natural reading behavior.
A website should also be easy to navigate. If a potential client finds themselves struggling to find the information they need, they’ll leave quickly. It’s also important to include a “contact us” page, allowing prospective clients to connect with your practice via phone or email.
Finally, a website should provide a clear listing of the services you offer. This allows prospects to easily compare your services with those of your competitors and helps you rank higher in location searches.
Convenience
A website allows you to showcase your work in a way that’s easy for potential customers and clients to find. You can also use it to educate people about your industry, which can help you build a following and gain trust in the community. This can ultimately lead to more sales and referrals.
Enhance your online presence with expert website design Seattle. A well-crafted website not only provides vital information like business hours and contact details but also streamlines customer interaction, reducing unnecessary calls and freeing up valuable employee resources. Let us optimize your website to maximize efficiency and productivity for your Seattle-based business.
Having a site also makes it easier for people with hearing or cognitive disabilities to navigate. It’s possible to create websites that accommodate these visitors by using clear language, font-pairings and limited color usage to convey meaning.
Portal websites are a great tool for businesses, schools and institutes, as they allow people to log in with a secure password and view their data like grades or schedules. It’s also a convenient place for people to interact with one another, as they can connect and share ideas via timelines and chats. Forums are another great example of a portal website, as they bring people with similar interests together and provide them with a common platform to discuss them. This type of collaboration increases productivity, which is why so many organizations are investing in portals for their employees and students.

Ease of Navigation
Website visitors are looking for information, and navigation is a big part of that process. Website navigation needs to be simple and straightforward to help guide users through the content on your website, from start to finish. This is an important component of good web design that should be considered carefully when planning a new site or redesigning an existing one.
Website navigation should be organized in a logical hierarchy that matches the way users are already used to navigating other websites. If your website is too complicated or your navigation doesn’t match users’ expectations, they will get frustrated and leave quickly. To avoid this, use a sitemap and breadcrumbs to orient your visitors and help them find what they’re looking for.
When your website has a clear, intuitive navigation system that meets users’ expectations, they will spend more time on your website—which means that they are more likely to convert from a visitor into a buyer. The three-click rule (named after the UX expert Jakob Nielsen) states that users will expect to be able to navigate from any page on your website to their desired destination within three clicks or less.
Your website should load fast, like a cheetah chasing its prey. A website that loads slowly will frustrate visitors and cause them to leave before they’ve even had a chance to search your site.
Visual Appeal
When it comes to digital marketing, visual appeal is a critical factor that influences consumers’ perception of products and brands, and ultimately their willingness to engage with them. This is especially true for websites, where visually appealing interfaces can amplify messaging and increase user engagement.
Creating an aesthetically pleasing website requires more than just an eye for detail; it also requires balance and consistency. A successful design uses whitespace to organize and emphasize content, uses font-pairings to communicate different messages, and creates a clear, intuitive navigation structure. It also includes a consistent color scheme, clean and inviting images, and simple, meaningful calls to action.
According to research by Lindgaard et al, visitors form their impressions of a website’s visual appeal within 50 milliseconds. They can reliably decide whether they like or dislike a page, and these first impressions hold up over time.
While achieving the perfect balance between aesthetics and functionality is a challenge, it is important for marketers to understand the role that visual appeal plays in online success. When a website has both visual appeal and ease of use, it establishes credibility and trust with users, making them more likely to convert to customers.



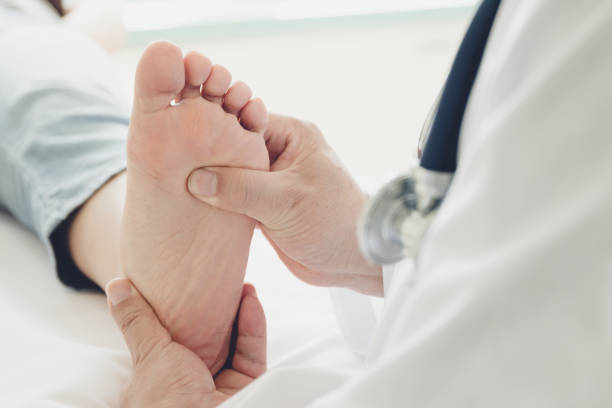

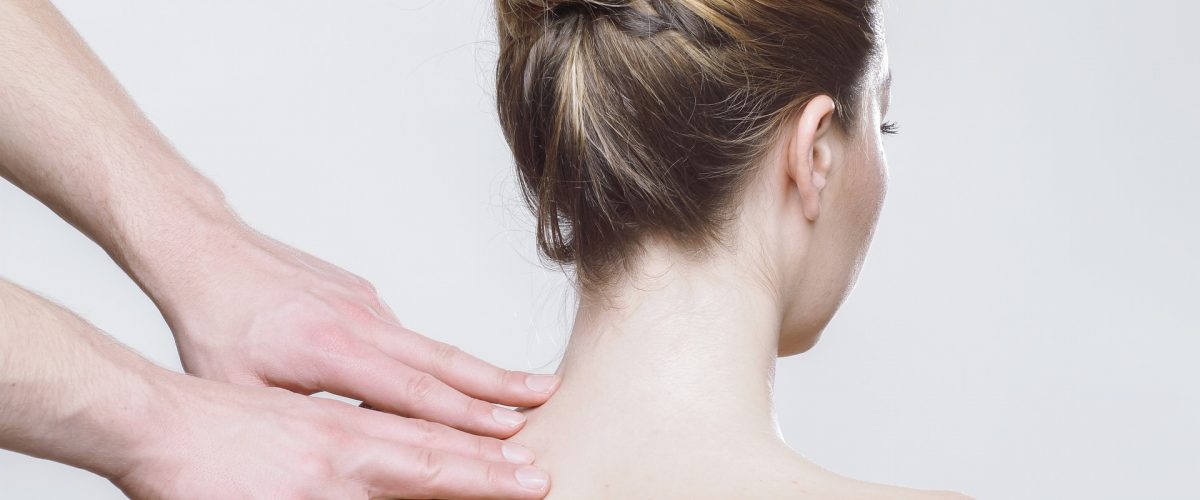
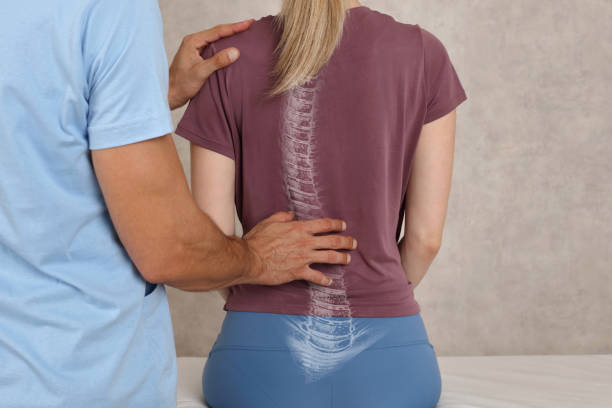 Osteopathy is a holistic medical practice that focuses on the body as a whole. It aims to bring about optimal blood flow and postural alignment. In addition, the therapy promotes a healthy lifestyle. This helps to reduce pain and discomfort and improve mobility.
Osteopathy is a holistic medical practice that focuses on the body as a whole. It aims to bring about optimal blood flow and postural alignment. In addition, the therapy promotes a healthy lifestyle. This helps to reduce pain and discomfort and improve mobility.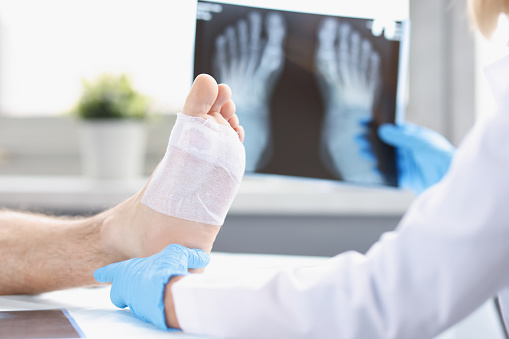
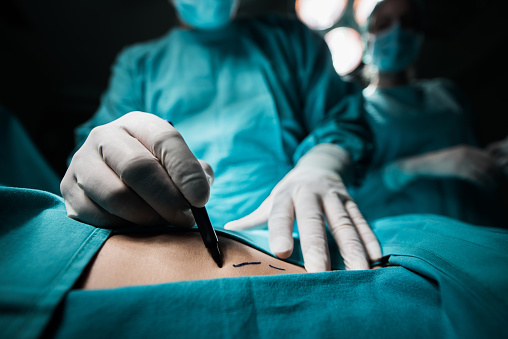
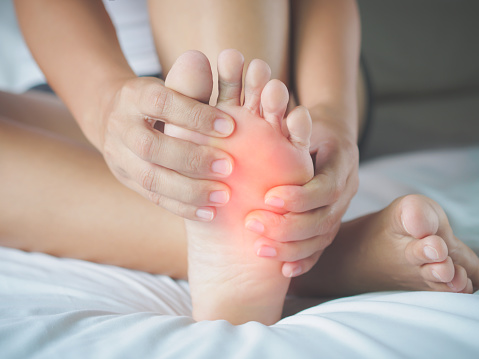
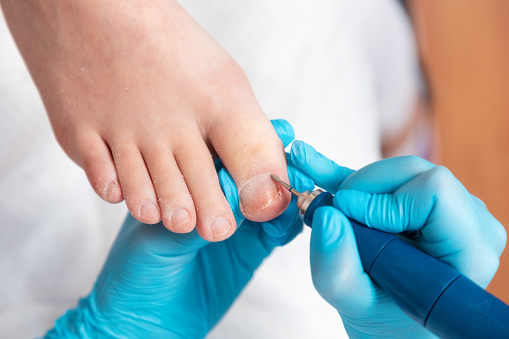 If you have an ingrown toenail, you may wonder whether it needs to be treated by a physician. There are several symptoms that can indicate an ingrown toenail, which can include pain and drainage of pus. If you notice any of these signs, you should see your doctor immediately. The best way to diagnose an ingrown toenail is to take a physical exam. You should also be careful to avoid pressure to the lateral nail fold.
If you have an ingrown toenail, you may wonder whether it needs to be treated by a physician. There are several symptoms that can indicate an ingrown toenail, which can include pain and drainage of pus. If you notice any of these signs, you should see your doctor immediately. The best way to diagnose an ingrown toenail is to take a physical exam. You should also be careful to avoid pressure to the lateral nail fold.
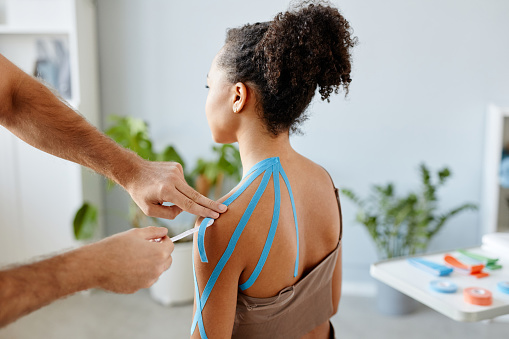


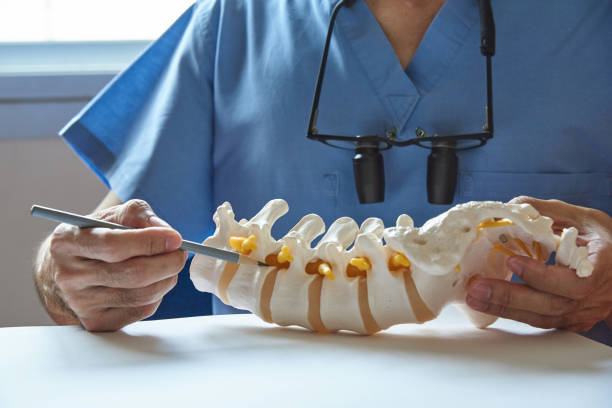
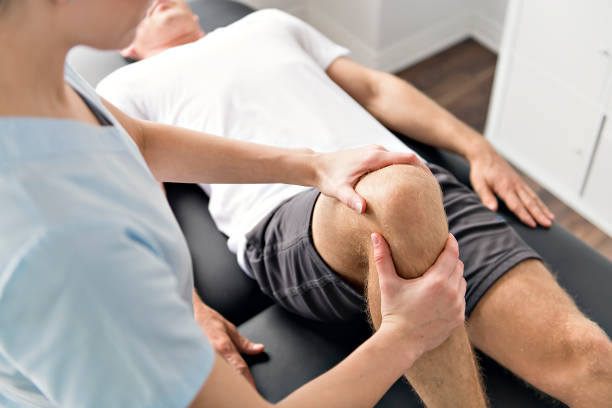
 If you’re suffering from back pain, your doctor may recommend you visit a chiropractor or a physical therapist. But what’s the difference between these two medical practices? Here’s an overview of what you need to know before making the decision. Both chiropractors and physical therapists use manual therapy as a treatment option. Both will assess your condition and your health history.
If you’re suffering from back pain, your doctor may recommend you visit a chiropractor or a physical therapist. But what’s the difference between these two medical practices? Here’s an overview of what you need to know before making the decision. Both chiropractors and physical therapists use manual therapy as a treatment option. Both will assess your condition and your health history.














 Are you having problems with your feet? Do you wake up with painful red spots, calluses, blisters, or other types of foot concerns? If so, it may be time to visit a podiatrist to have your feet looked at. Most people think that a chiropractor will only work on their back, but a few podiatrists now offer services that can range from keeping your feet healthy and free of pain to actually diagnosing problems that may be causing the pain.
Are you having problems with your feet? Do you wake up with painful red spots, calluses, blisters, or other types of foot concerns? If so, it may be time to visit a podiatrist to have your feet looked at. Most people think that a chiropractor will only work on their back, but a few podiatrists now offer services that can range from keeping your feet healthy and free of pain to actually diagnosing problems that may be causing the pain.